Instant Access
SMS-first engagement—no portals or app downloads for members
Seemless Integration
Integrates seemlessly with existing management platforms
Private & Secure
Enterprise-ready privacy and compliance integration
IDENTIFY who needs support now by assessing risks, gaps and rising acuity
ENGAGE with members proactively via SMS and workflows
RESOLVE barriers fast with closed-loop navigation and follow through
IMPACT proven through clear reporting tied to quality and utilization
QUALITY performance through HEDIS/Stars-related gaps and adherence support

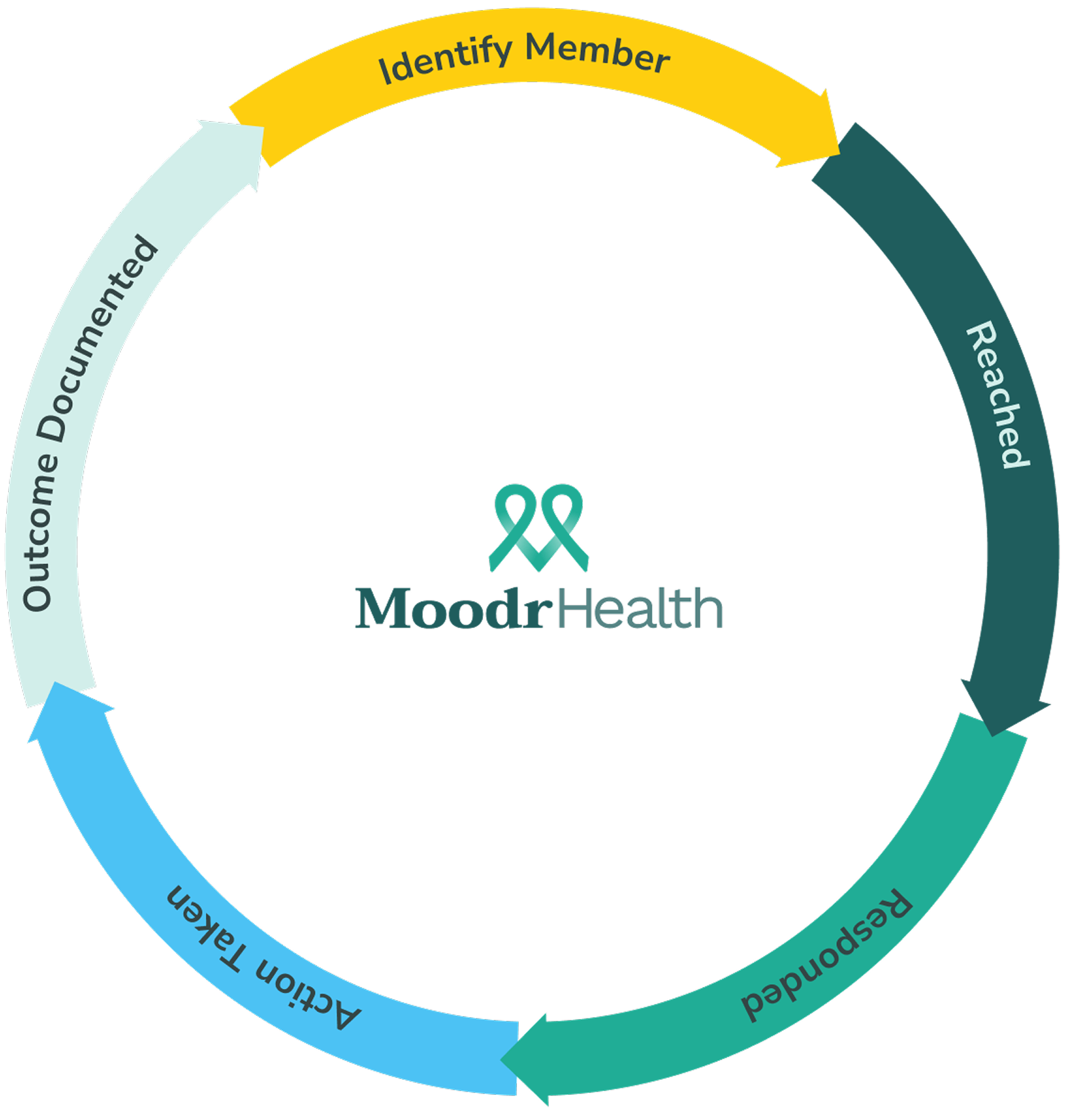
A Repeatable Team-run Engagement Workflow
Moodr is a SMS-first engagement layer that helps your care management and member services teams move members through a close-loop tracking at every step.
1) Connect to your existing systems
Moodr integrates with your current CRM, care management tools, and data feeds so you can activate outreach from the sources you already use.
2) Identify
Target members based on risk, gaps, rising acuity, program criteria, or simple lists and segment them by population, program, or priority.
3) Engage
Launch compliant SMS outreach with configurable message flows, timing, and routing that is built for real-world response patterns.
4) Route & Resolve
Guide next steps through structured workflows schedule, complete screening, connect to services, create referrals, or escalate to a care manager.
5) Close the Loop
Track follow-through and document resolution so you’re not just “sending messages”, but instead you’re proving communication and action is taking place.
Measurement that Ties Activity to Performance
Reach & Response
See delivery, patient response rates, and provider time-to-respond
Conversions
Track who enrolls, schedules, completes screenings, or accepts referrals
Follow-through
Follow completion rates, drop-off, and closed-loop resolutions
Audit-ready Records
Access structured documentation of outreach and outcomes
Program Performance
Stats about populations, regions, vendors, clinics, or cohorts
High-impact Plan Use Cases
Care Management Enrollment
Increase opt-ins and reduce drop-off with automated follow-ups
Quality Gap Closure
Reminders and guided actions for screenings, labs, preventive care, adherence
Maternal Health
PMAD screening, perinatal SUD outreach, ongoing check-ins, escalation pathways
Behavior Health Management
Retention, touchpoints between visits, risk escalation workflows
SDOH Navigation
Needs are captured, referral is made, confirmation of connection solidified and then have access to resolution tracking
Your teams can run consistent engagement programs at scale and prove impact in a way that leads to quality and utilization.
From Pilot to Statewide Rollout
Aetna Better Health of West Virginia piloted Moodr with six “super‑users” to improve enrollment into care management plans. The goal was a 15% increase in care-plan enrollment and the results came in closer to 57% increase in care-plan enrollment. Following the pilot, Aetna expanded Moodr to additional care managers statewide, using SMS-first outreach as part of a measurable enrollment workflow.

